During a flare, start with clear liquids, then low fiber foods before gradual fiber.
If you are wondering what to eat with diverticulitis, you are not alone. I have guided many clients through flares and long-term recovery. In this guide, I break down what to eat with diverticulitis at each stage, backed by clinical practice and current research, so you can feel better with confidence and a plan.

Understanding diverticulitis and how food helps
Diverticulitis is inflammation or infection of small pouches in the colon. During a flare, the gut needs rest, then gentle foods, and later, fiber to support healing. Knowing what to eat with diverticulitis at each phase can reduce pain, lower risk of complications, and help prevent future flares.
What matters most is timing. During a flare, you simplify. During recovery, you rebuild. When you are well, you focus on fiber, fluids, and steady habits.

What to eat with diverticulitis during a flare
When pain is sharp, you need calm. Most people start with a clear liquid diet for 24 to 48 hours, unless a clinician advises otherwise. This approach lowers residue in the colon and may ease symptoms.
Try these clear liquids when symptoms peak:
- Water, oral rehydration solution, or diluted sports drinks
- Clear broths, strained soups, or bone broth
- Plain gelatin, ice pops without pulp, or electrolyte ice
- Weak tea or decaf coffee without cream
As pain drops and you feel hungry, move to low fiber, soft foods:
- White rice, plain pasta, cream of wheat, or white toast
- Scrambled eggs, tofu, smooth nut butters in small amounts
- Plain yogurt, kefir, cottage cheese
- Canned peaches or pears without skin, applesauce, mashed potatoes without skin
Protein matters for healing. Choose gentle sources like eggs, fish, tofu, and tender chicken. Keep fat low at first to avoid cramps.
I ask clients to follow a simple 3-step flow for what to eat with diverticulitis:
- Clear liquids for 24 to 48 hours, if pain and fever are present
- Low fiber, soft foods for 2 to 3 days as symptoms improve
- Return to a balanced, higher fiber plan once you are pain-free and regular
:max_bytes(150000):strip_icc()/VWH-MiraNorian-LiquidDietforDiverticulitis-Standard-5e54993412734a5b9dec5e34927a5700.jpg)
Transition after a flare: rebuilding fiber safely
When pain settles, begin to add soluble fiber first. Soluble fiber forms a gel and is easier on the gut. Great choices include oatmeal, barley, ripe bananas, canned fruit in juice, sweet potatoes without skin, and psyllium as advised.
Advance slowly. Add one higher fiber food per day and watch for bloating or cramps. If gas rises, pause and try again in two or three days. This gentle ramp works better than a fast jump.
Probiotic foods can help some people. Yogurt with live cultures, kefir, miso, and sauerkraut in small amounts are good options. If you are unsure, ask your clinician before starting a supplement.
Using a journal helps. Note what you ate, symptoms, and timing. Over a week, you will see your personal pattern for what to eat with diverticulitis during recovery.

Long-term pattern to prevent recurrence
When you feel well, fiber is your friend. Aim for about 25 grams per day for most women and 38 grams for most men. Increase by 5 grams per week until you reach your goal, and drink more water as fiber goes up.
Build your plate around:
- Vegetables and fruit, fresh or cooked, with skins if you tolerate them
- Whole grains like oats, brown rice, quinoa, and whole wheat
- Legumes like lentils, chickpeas, and black beans, cooked very soft at first
- Nuts and seeds, added slowly, as most large studies show they do not trigger flares
Balance matters. Limit processed meats, sugary snacks, and excess alcohol. Regular movement, stress care, and sleep also help lower flare risk.
People often ask if seeds and popcorn are off the table. Evidence does not support that rule for most people. Focus instead on total fiber, variety, and your own tolerance.

Sample 3-day meal path you can follow
This plan shows what to eat with diverticulitis across the flare, transition, and long-term stages. Adjust portions to your needs and clinical advice.
Day 1: Flare easing, low fiber
- Breakfast: Cream of wheat with a spoon of honey; weak tea
- Lunch: Clear chicken broth; white toast; applesauce
- Snack: Plain gelatin or an electrolyte ice
- Dinner: Scrambled eggs; white rice; canned peaches in juice
Day 2: Transition, add soluble fiber
- Breakfast: Oatmeal made soft; ripe banana; water
- Lunch: Baked potato without skin; low fat cottage cheese
- Snack: Yogurt with live cultures
- Dinner: Poached salmon; soft carrots; white rice moving toward brown
Day 3: Stable, higher fiber
- Breakfast: Overnight oats with chia; blueberries if tolerated
- Lunch: Lentil soup, well cooked; whole grain toast
- Snack: Apple with skin if tolerated; small handful of almonds
- Dinner: Chicken, quinoa, roasted zucchini; side salad if tolerated

Hydration, supplements, and medications
Hydration is key in every phase. A simple goal is pale yellow urine. Most adults need about 2 to 3 liters per day, more if the weather is hot or if you are active.
Fiber supplements can help, but timing matters. Psyllium can support regularity when you are stable. Do not add fiber supplements during a severe flare without medical guidance.
Probiotic supplements have mixed evidence. Some people feel better; others see no change. Start low, track your response, and talk with your clinician.
For pain, acetaminophen is often preferred. Many clinicians ask you to avoid nonsteroidal anti-inflammatory drugs if possible, as they may irritate the gut. Antibiotics are not always needed for mild, uncomplicated flares, but follow your doctor’s plan.
If you keep asking yourself what to eat with diverticulitis, remember this trio: fluids, gentle fiber, and steady steps.

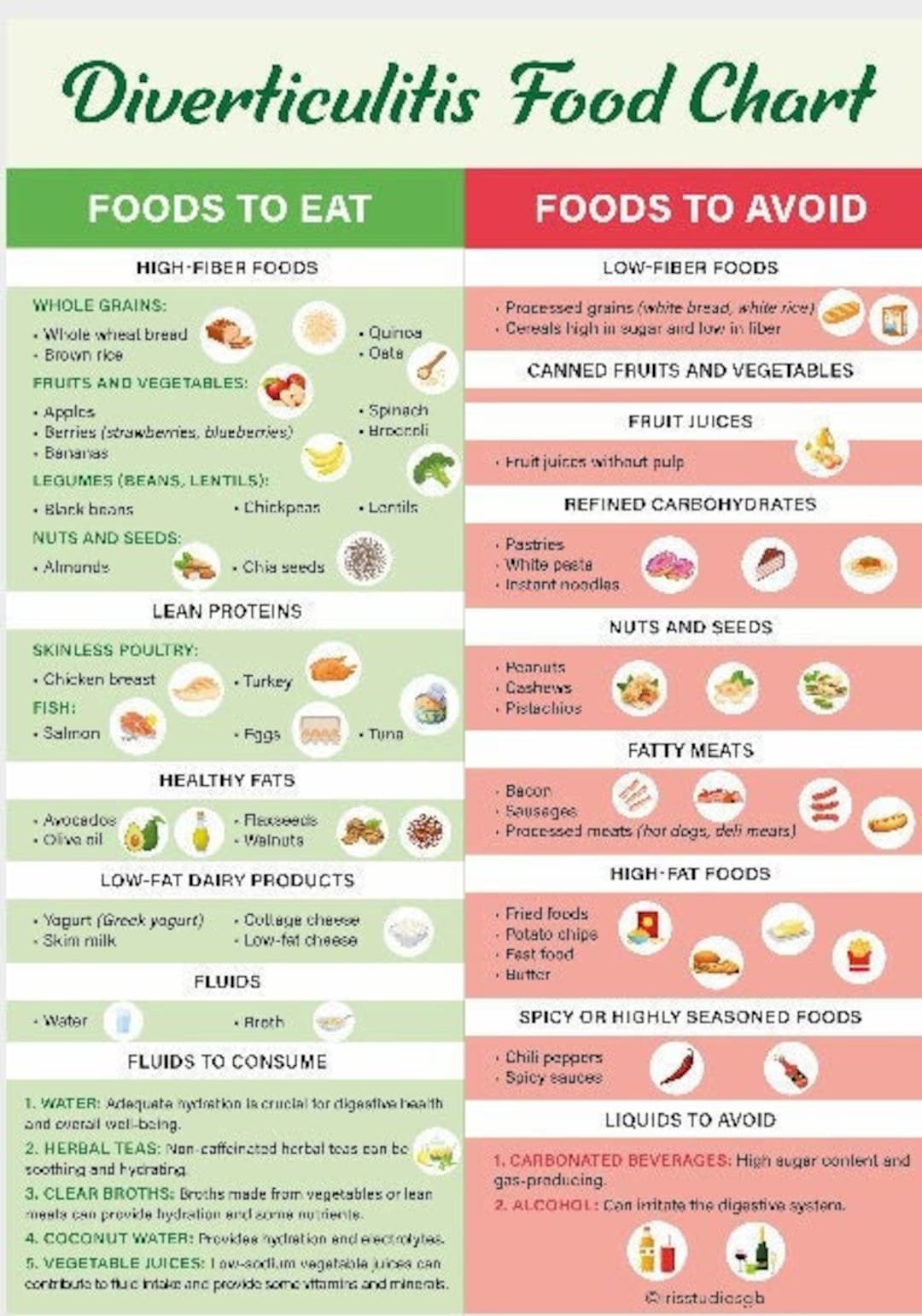
Foods to limit or avoid
During a flare, skip high fiber and rough textures. These can be hard to digest and may worsen pain. When you are well again, most foods can come back.
Limit during a flare:
- Raw veggies and large salads
- Tough meats and fried foods
- Whole nuts, large seeds, and popcorn
- Alcohol, high caffeine, and fizzy drinks
Limit long-term:
- Processed and red meats
- Refined grains and sugary snacks
- Heavy alcohol and smoking
Spicy food does not cause diverticulitis, but it can trigger symptoms in some people. Test small amounts and see how you feel. Keep your plan centered on what to eat with diverticulitis that supports comfort and fiber balance.
Shopping, cooking, and eating out tips
Build a small “flare kit” at home. Having the right foods on hand makes a hard day easier. I keep clients ready with a shelf box and a freezer plan.
Smart pantry picks:
- Broths, gelatin, oral rehydration packets
- White rice, pasta, oatmeal, cream of wheat
- Applesauce, canned peaches and pears in juice
- Canned salmon and tuna, yogurt, kefir
Cooking tips:
- Use moist heat like braise, steam, or poach
- Peel and cook veggies well in early recovery
- Batch cook soups and freeze in small portions
Dining out:
- Choose baked or grilled proteins
- Ask for soft sides like rice or mashed potatoes
- Request sauces on the side and skip raw salads early on
If you are unsure what to eat with diverticulitis while traveling, pack shelf-stable options like oatmeal cups, applesauce pouches, and oral rehydration packets.

When to seek care and safety notes
Diet is important, but it is not the whole story. Call your clinician if you have fever, severe or one-sided lower belly pain, rectal bleeding, vomiting, or you cannot keep liquids down. Go to urgent care if pain worsens or you feel faint.
High risk groups need closer follow-up. This includes people with immune issues, kidney disease, or steroid use. Ask your doctor for a written plan that includes what to eat with diverticulitis at each step, plus when to use medicines and when to call.
Every gut is unique. Adjust these steps with your care team. If a food hurts, pull back, wait, and try again later.
Frequently Asked Questions of what to eat with diverticulitis
Can I eat nuts and seeds?
Most people can enjoy nuts and seeds when they are well. Large studies show no higher risk of flares from these foods. Start small and chew well.
Do I need a low fiber diet forever?
No. Low fiber is for the flare phase only. Long-term, a higher fiber diet helps prevent future flares.
Are probiotics helpful for diverticulitis?
They may help some people, but results are mixed. Try food sources first and track your response. Speak with your clinician before starting a supplement.
Is coffee safe to drink?
Many people tolerate coffee in recovery and long-term. During a flare, choose weak tea or decaf to reduce cramps.
What about alcohol?
Alcohol can irritate the gut and raise flare risk for some people. Avoid during a flare and limit long-term.
Should I follow a low FODMAP diet?
Low FODMAP can reduce gas and bloating for some with IBS. It is not a standard plan for diverticulitis but can be used short term under guidance.
Can I eat popcorn again?
Yes, most people can bring back popcorn when they are symptom-free. Start with a small amount and see how you feel.
Conclusion
You now have a clear, step-by-step plan for eating through a flare, a safe recovery, and strong long-term habits. Start with clear liquids, shift to low fiber as pain fades, then build a fiber-rich plate with plenty of fluids and steady routines. Small, steady changes add up to fewer symptoms and more good days.
Use the ideas here to map out your own plan this week. Keep a simple journal, stock your flare kit, and set a daily fiber goal. Want more helpful guides like this? Subscribe, share a comment with your questions, and let me know which meals worked best for you.

